Airway surface hyperviscosity and defective mucociliary transport by IL-17/TNF-α are corrected by β-adrenergic stimulus
Authors: Daniela Guidone, Martina Buccirossi, Paolo Scudieri, Michele Genovese, Sergio Sarnataro, Rossella De Cegli, Federico Cresta, Vito Terlizzi, Gabrielle Planelles, Gilles Crambert, Isabelle Sermet, and Luis J.V. Galietta
Year: 2022
Sources: JCI Insight
Abstract:
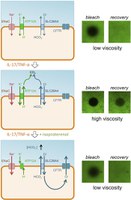
The fluid covering the surface of airway epithelia represents a first barrier against pathogens. The chemical and physical properties of the airway surface fluid are controlled by the activity of ion channels and transporters. In cystic fibrosis (CF), loss of CFTR chloride channel function causes airway surface dehydration, bacterial infection, and inflammation. We investigated the effects of IL-17A plus TNF-α, 2 cytokines with relevant roles in CF and other chronic lung diseases. Transcriptome analysis revealed a profound change with upregulation of several genes involved in ion transport, antibacterial defense, and neutrophil recruitment. At the functional level, bronchial epithelia treated in vitro with the cytokine combination showed upregulation of ENaC channel, ATP12A proton pump, ADRB2 β-adrenergic receptor, and SLC26A4 anion exchanger. The overall result of IL-17A/TNF-α treatment was hyperviscosity of the airway surface, as demonstrated by fluorescence recovery after photobleaching (FRAP) experiments. Importantly, stimulation with a β-adrenergic agonist switched airway surface to a low-viscosity state in non-CF but not in CF epithelia. Our study suggests that CF lung disease is sustained by a vicious cycle in which epithelia cannot exit from the hyperviscous state, thus perpetuating the proinflammatory airway surface condition.
Category: journals